Inside This section
Athletic Injuries to the Leg, Foot and Ankle
History
The first recorded athletic injury appeared in Genesis 32:24-24…
“So Jacob was left alone, and a man wrestled with him till daybreak. When the man saw that he could not overpower him, he touched the socket of Jacob’s hip so that his hip was wrenched as he wrestled with the man.”
Galen (second century AD) was first sports physician to the gladiators.
Epidemiology
Sports injuries are incredibly common and most occur in the lower limb. There are estimated 350 ankle sprains in Sydney each day.
Chronic Leg Pain
Well known list of differential diagnoses in decreasing order of frequency…
- Chronic compartment syndrome
- Medial tibial stress syndrome
- Stress fractures
- Gastrocnemius strain
- Nerve entrapment syndromes
- Venous disease
- Arterial occlusion
- Fascial herniation
- Tendonitis Radiculopathies
Diagnosis is often helped by history and examination.
Chronic
A muscle that swells in it’s confined fascial space. Most common in the anterior compartment, followed by deep posterior, lateral and superficial posterior (Martens and Meyersons Sports Med. 9:62 1990).
Diagnose with measurement of resting and exertional pressures.
Chronic Compartment Syndrome
A muscle that swells in it’s confined fascial space. Most common in the anterior compartment, followed by deep posterior, lateral and superficial posterior (Martens and Meyersons Sports Med. 9:62 1990).
Diagnose with measurement of resting and exertional pressures.
Criteria
- A good history
- Resting Pressure > 15 mmHg (Normal 0 – 8)
- An exercise pressure > 75 mmHg is diagnostic
- 1 min post exercise > 30mmHg
- 5 – 10 min post exercise > 15 mmHg
Treatment
Live with the pressures or have a fasciotomy.
Medial Tibial Stress Syndrome
A stress reaction alone with the postero-medial aspect of the tibia variously attributed to the fascia, periosteum or bone. A heterogeneous entity which may involve the attachment of soleus, periostitis beneath the tibialis posterior, a stress reaction on the tibia or even the flexor digitorum longus muscle overuse.
Diagnose with a bone scan and do not confuse with deep posterior compartment syndrome.
Treatment
Modification of activities, NSAIDS. Role of surgery is controversial. Most surgical proponents combine a deep posterior fasciotomy with release of the fibrous arch of the soleus and claim 80% good or excellent results (Jarvinnen et al. Int. J. Sports Med. 10:55. 1989).
Gastrocnemius-Soleus Strain
Occurs in middle aged tennis players who suddenly extend their knee with their ankle in full dorsiflexion. Manage with initial rest the stretching and strengthening to regain function.
Nerve Entrapment Syndromes
Superficial peroneal the most common. Most nerves have been described such as posterior tibial, saphenous, sural and common peroneal as it transverses the neck of the fibula. Patients will describe a pain that is burning, tingling and often radiating.
Treatment
Local therapy such as NSAID creams, amytryptyline, surgical release combined with fasciotomy.
Popliteal Artery Entrapment Syndrome
A relatively rare entity that causes pain in athletic individuals. Cause is anatomical variations in the course of the popliteal artery leading to compression. Delaney and Gonzalez Surgery 69:96 1971). May be difficult to differentiate from exertional compartment syndrome. May produce a picture similar to intermittent claudication.
Diagnose with bi-planar arteroigraphy performed after exercise.
Lateral Ankle And Ligament Injury
The most common orthopaedic injury. One per 10,000 population per day, ie 350 in Sydney today!
Ligaments involved are the anterior talo-fibular ± the calcaneofibular. Bostrum believed that isolated tears of the calcaneofibular ligament were very rare.
Mechanism of injury is a plantar flexion-inversion sprain.
Grade As
I – Stretch
II – In between I and III
III – Complete rupture
Treat all non-operatively in my opinion (no significant difference between cast, operative repair and controlled early mobilisation) looking at re-injury, functional instability, range of motion, pain/swelling/stiffness, return to pre-injury activity.
Rest Ice Compression Elevation works well – non weight bearing with crutches or weight bearing in an aircast(r) brace for the first few days, the range of motion exercises and proprioceptive retraining.
Of interest is that the subjective and objective stability don’t correlate.
Outcome In Military Recruits
Grade I – 8 days
Grade II – 15 days
Grade III – 21 days +
In workers compensation double these times.
Chronic instability is easily dealt with by delayed ligament reconstruction with > 90% good results
Sources Of Continuing Pain Or Instability After Ankle Sprain
Articular Injury
- Chondral fractures
- Osteochondral fractures
Nerve Injury
- Superficial peroneal
- Posterior tibial tendon
Tendon Injury
- Peroneal tendon (tear or dislocation)
- Posterior tibial tendon
Other Ligamentous Injury
- Syndesmosis
- Subtalar
- Bifurcate
- Calcaneocuboid
Impingement
- Anterior tibial osteophyte
- Anterior inferior tibiofibular ligament
Miscellaneous Conditions
- Failure to regain normal motion (Tight TA)
- Proprioceptive deficits
- Tarsal coalition
- Meniscoid lesions
- Accessory soleus muscle
- Normal X-Ray does not equal normal ankle.
- Current Concepts review on ankle sprains: JBJS 73A, 305 1991.
Osteochondral lesions of the talus
- Also known as osteochondral fractures of the talus, talar dome lesion, osteochondritis dissecans.
- Aetiology – trauma or spontaneous osteonecrosis?
Incidence
- 9% of “chronic ankle sprains”
- Medial > lateral
- Age 20 – 30
- Bilateral about 10%
Location (Ferkel)
- Medial are mid or posterior 1/3 and deep
- Lateral are mid or anterior 1/3 and shallow
Classification Modified (Berndt and Hartly JBJS 41a:988. 1959)
- X-ray based though appearance at arthroscopy/CT or MRI is more useful
- I Small trabecular compression fracture without displacement
- II Partially detached osteochondral fragment (IIA Cyst formed)
- III Fully detached osteochondral fragments remaining in its bed
- IV Completely detached fragment of loose body
Diagnosis
- Plain x-rays are usually normal – therefore Clinical Suspicion Bone scan then CT or MRI.
- CT scan image of a cyst in the talus may be traumatic and indicates chronicity – see image below…
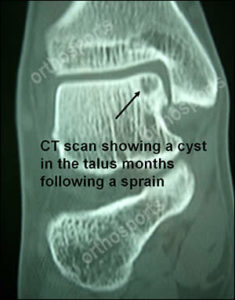
Treatment
- Arthroscopic treatment a great advance
- Unroof lesion, curette out loose fragments
Post Operative
- NWB 2 weeks if lesion < 1.5cm
- NWB 6 weeks if lesion > 1.5cm
Read Anderson et al JBJS 71A:1143. 1989. (Good Australian paper)
Anterolateral Gutter Synovitis / Impingement
- Described by Wolin in 1950.
- Recently popularised by Richard Ferkel of Van Nuys California.
The Sequence Of Events Postulated Is:
- Inversion sprain
- Torn ATFL
- Incomplete healing
- Repetitive motion
- Inflamed ligament ends
- Synovitis
- Scar tissue
- Impingement
- Chronic ankle sprain
Treatment
- Physiotherapy
- Immobilisatio
- Cortisone injection
- Arthroscopic debridement
Results
- Ferkel claims 84% good or excellent results in 75 patients with >2 year folow-up.
- The most common foot and ankle fracture.
There are essentially two types:
1. Tuberosity fractures – very common
2. “Jones” fractures – less common
Tuberosity fractures may or may not involve the 5th tarsometatarsal joint. Theories of aetiology include peroneus bevis avulsion and avulsion by the lateral fibres of the plantar ligament.
Most patients will give the history of an inversion injury.
Management is symptomatic. I recommend either a post-operative shoe or an aircast weightbearing. If the patient is in too much pain to weight-bear then a period non-weightbearing on crutches is suggested. Disability rarely lasts longer than 6 weeks. Non-union is rarely a problem as fibrous pseudoarthrosis is usually painless. For a displaced intra-articular fracture surgery should be considered.
The Jones Fracture
Named after Robert Jones who in 1902 described a fracture he sustained whilst dancing (approximately three-quarters of an inch from the fifth metatarsal base”. He made no comment on the preferred method of treatment though stated that his disability was considerable. Vascular studies have shown this area to be a watershed and therefore the incidence of delayed/non union is explained.
Jones Fracture Management
The acute fracture is best treated initially with six weeks non-weightbearing in a cast. The majority of “fresh” fractures will heal with this regime. If union fails to occur then intramedullary fixation with a screw and a bone graft is suggested.
Achilles Tendon Rupture
A common injury that is surprisingly frequently missed. Acute rupture most common in males between the ages of 30 and 50 “Weekend warriors” more often than trained athletes though not always the case. Painful prodrome is volunteered if asked.
Diagnosis
Obvious? No! 25% are missed by the first treating physician.
History is characteristic and involves a sudden severe pain in the back of the ankle “like being struck with a tennis ball” with or without an associated loud pop.
Physical examination – feel for the gap.
Thompson or Simmonds test.
CAUTION: DO NOT TRUST ULTRASOUND OR MRI… THE DIAGNOSIS IS CLINICAL.
The slide below shows a complete rupture of the achilles tendon at surgery – the ultrasound was reported as showing a partial tear.
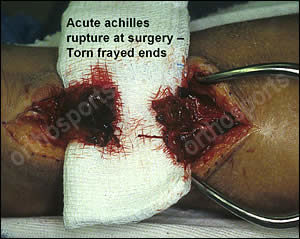
Treatment
Controversy existed regarding operative vs Non-operative treatment. The considerations include ultimate strength, length, re-rupture and the sometimes disastrous complications of surgery. In general surgical reconstruction is favoured as the rate of re-rupture is less and the functional length of the tendon is easier to restore. In young athletic patients the re-rupture rate following non-operative treatment is unacceptable (10% vs 2%).
The rehabilitation is undergoing change and a trend is developing towards earlier mobilisation with better outcomes with respect to strength and rates of re-rupture.
Chronic TA Rupture or Missed TA Rupture
Indications for surgery are persistent pain and weakness. The operative procedures are not without their morbidity and all operations are a compromise.
Relative Strength Of Muscles
- Gastroc-soleus 49.1
- FHL 3.6
- Penroneus Brevis 2.6
- FDL 1.8
Described in the last 15 years
Thought due to mechanical overload
Presents with associated instability of the joint
Diagnosis is clinical
Think of associated arthropathy (Seronegative in young males)
Treatment
- Tape the toe
- NSAIDS
- 3/4 length insole metatarsal dome
- Judicious use of steroid injection
- Surgery
Far more common than pilon fractures and also much easier to treat. The mechanism of injury varies and was elegantly described in Lauge-Hansen in his classic series of articles in the 1950’s. The commonest ankle fracture is the so-called supination external rotation injury. The first word (supination) describes the position of the foot and the subsequent movements (external rotation), the mechanism of injury. Other common mechanisms are pronation-abduction and supination-abduction. These particular injuries produce characteristic fracture patterns according to the degree of injury.
Classification Of Ankle Fractures
The Dennis-Weber Classification is the most commonly used system because it is easily recalled, it pertains to the relation ship of the fibular fracture to the syndesmosis…
A – Below the syndesmosis
B – At the syndesmomsis
C – Above the syndesmosis
Treatment Principles
The AO group has dominated thinking about ankle fractures for the last 20 years. The fibular has been the focus of attention with early biomechanical work stating it’s weight-bearing role and the detrimental effects of even small alterations in it’s position (Ramsey and Hamilton [ii]).
Such an approach behooves the surgeon to operate on almost every ankle fracture as displacements of even 1 mm are not tolerated. Recent research is giving the medial side greater prominence and suggests that earlier concepts of the fibular as the main stabiliser of the ankle were erroneous (iii). Indeed, syndesmotic injury in the absence of medial injury has been shown not to affect talar displacement in a cadaver model (iv)
1. With an intact medial side no advantage has been shown (operative vs. Non-operative) in the management of isolated fractures of the lateral malleolus.
2. In bi-malleolar fractures, an anatomical reduction has been shown to correlate best with a successful outcome. This is of course most easily achieved surgically according to AO principles of rigid internal fixation with early joint mobilisation.
3. In Weber C injuries (with medial disruption) a syndesmotic screw should be considered in injuries > 3 cm above the plafond. Use a 4.5 mm screw engaging 3 or 4 cortices and not lagged.
4. In posterior malleolar fractures involving > 25% of the joint, anatomical reduction is recommended. I prefer the posterolateral approach with the patient in the lateral decubitus position.
I – Lauge-Hansen N, Fractures of the ankle II. Combined experimental-surgical and experimental-roentgenologic investigations. Arch Surg 69: 957-985. 1950.
II – Ramsey PL Hamilton W, Changes in tibio-talar area of contact caused by lateral shift. JBJS 58A: 356, 1976.
III – Michelson JD, Current concepts review, Fractures about the ankle. JBJS 77A, 142. 1995.
IV – Boden SD, Labropoulos PA, McCowin P, Lstini WF, and Hurwitz SR, Mechanical considerations for the syndesmosis screw JBJS 71A: 1548. 1989.
