Home > Teaching > Injection Techniques > Knee Injections
Knee Injections
Injecting the knee is an important part of general practice, rheumatology and sports medicine. The technique and the indications are discussed below. Its application not only helps confirm certain diagnosis but also treat some common conditions. Below you will find the most common reasons for injecting the knee and this will hopefully make you more confident in doing so.
Local anaesthetic is useful to make certain diagnoses. It can be used alone or mixed with corticosteroid. Short acting agents include lignocaine, whilst longer acting agents include Naropin and Marcaine. There are certain toxic doses but these are unlikely to be exceeded in general practice. If in doubt, consult the product information sheet.
REMEMBER, if you stick a needle into something you think might be infected, send a specimen away for microscopy, culture and sensitivities.
Corticosteroid injections are used to relieve symptoms of arthritis in certain joints and are also used to reduce soft tissue inflammation. The appropriate use and knowledge of where and when to inject is extremely important.
To view Dr Doron Sher’s Knee Injection technique video please Click Here
Indications for Local Anaesthetic Alone
- Suturing a wound
- Diagnosis of pain coming from a certain part of the knee, e.g., bursa, iliotibial band. This is not common and usually should be done by a surgeon or sports physician.
Corticosterioids act as an anti-inflammatory medication which can be injected into a joint or around some tendons (use with caution around tendons). Corticosteroid is usually mixed with local anaesthetic to reduce pain which is usually only quite mild.
When is it used?
There are multiple indications and we will discuss the most common ones. In general it is used to relieve inflammation of tendons or joints.
Intraarticular Injection
Intra-articular corticosteroids are primarily used for pain secondary to osteoarthritis but they can also be used in inflammatory conditions such as rheumatoid arthritis. They do not slow down or change the progression of arthritis.
They are generally used in patients with arthritic symptoms who are not symptomatic enough to warrant a total joint replacement. It is also used when trying to delay an inevitable joint replacement.
They are also useful in patients who are not medically fit for surgery.
How long does it last?
The effects usually take 24-48 hours to work. For the first day or two there can actually be a slight increase in pain as the corticosteroid starts to work. The effects can last anywhere from a week to 6 months but it is only temporary. You can repeat the injections if required (up to three a year).
Where is it Done?
Corticosteroids can be injected into the knee in the office under aseptic conditions.
Contraindications
- Suspected infection in the joint
- Cellulitis
- Immunosuppression
- Allergy to local anaesthetic or steroids
- Joint replacement (relative)
Side effects are rare…
Side Effects
- Risk of infection is low ( about 1 in 5000)
- Skin discoloration
- Fat necrosis
- Flare up of symptoms for a day or two
- Rise in sugar levels in diabetics- need to monitor levels carefully for about two days
Technique
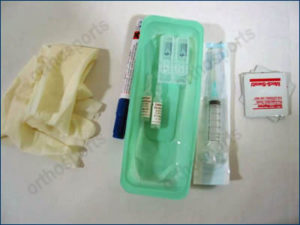
The choice of steroid varies. Celestone is one of the more common steroids used. Mix 2 ampoules of Celestone with 3 mls of local anaesthetic (lignocaine) in a 5ml syringe. Mix using an aseptic technique and use a blue or green (21,23G) needle. The choice of injection portal is either superolateral under the patella with the knee extended or through the inferomedial or inferolateral soft part of the knee with the knee flexed to 90 degrees. Always use an aseptic technique.
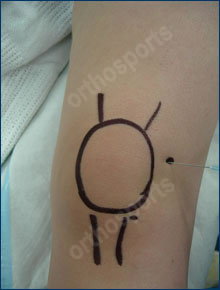
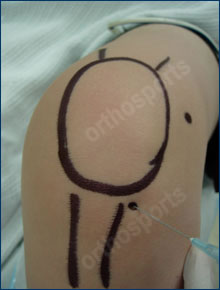
You do not need to aspirate the knee first unless there is a large effusion. If you do aspirate send the fluid off for culture.
Other parts of the knee which may need to be aspirated or injected include the prepatella bursa. This is superficial to the patella and can be traumatic or infective. If you think it might be infected, aspirate heading straight down toward the patella, not into the knee joint. You should not be able to go into the joint because you will hit bone first.
Other bursae or fluid collections do occur. Aspiration or injection should only be done if you are sure of the diagnosis, otherwise you should seek an orthopaedic opinion. A Bakers cyst is extremely common and should not, as a general rule, be aspirated.
