Home > Teaching > Newsletter > 2006 Newsletter – Summer
2006 Newsletter - Summer
Dear General Practitioners,
Welcome to our second Newsletter of the year and thank you for all the positive feedback from the last one. We are hoping to continue with our newsletter twice a year and would love to hear which topics you would like discussed. We have an extensive list of general practitioners but if you change address or wish to be removed from our mailing list please let us know.
Orthosports is pleased to announce that we are opening a new office on Macquarie Street in the city. This will take place in early December and involve both Orthopaedic surgeons and sports medicine physicians. Doctors Popoff, Sher and Walker will consult from these rooms covering hip, knee, shoulder and elbow surgery. There are X-ray and pathology services available in the same building and our contact details are listed below. Of course appointments can also be made through and for any of our other offices. The new office will allow your patients to be seen in a timely manner at a location more convenient for them. If surgery is required this can be arranged at a number of locations in Eastern, Western and Southern city for both public and private patients. We are happy to discuss patient care and take urgent referrals.
New City Office Opening
Address:
Park House, 2nd Floor,
187 Macquarie Street, Sydney
Phone:
(02) 9233 2883
Below is some more information on common Orthopaedic conditions which you may treat. If you have any particular requests for certain topics, please email or contact the rooms. The past newsletters and much more educational information are present on this website.
Swimmers/Surfers Shoulder
Swimmers or Surfers Shoulder is a common condition affecting both competitive and recreational swimmers and surfers. It is basically an overuse injury which results in the patient presenting with impingement or rotator cuff type symptoms.
The primary pathology is muscle imbalance. The freestyle and surfer’s strokes result in overdevelopment of the internal rotators and the anterior chest wall musculature. The end result is that scapula assumes a protracted, abducted position with associated reduction in the subacromial space. This, combined with the relative weakness of the infraspinatus, leads to impingement of the supraspinatus tendon on the under surface of the Acromion. The swelling associated with repeated impingement leads to further reduction of the subacromial space.
With time the abnormal scapula position becomes relatively fixed secondary to tight anterior structures. If left untreated the patient suffers continuing disability and risks the development of supraspinatus tendinosis or a tear.
Diagnosis – The diagnosis is usually straight forward. The patient complains of anterior shoulder pain during or after activity. On examination they often have scapula malpositioning resulting in a round shouldered appearance and slight winging. Tenderness over the supraspinatus insertion into the greater tuberosity is common. A painful arc is often present in forward flexion and abduction, and impingement tests are positive.
Treatment – Treatment involves correction of the muscle imbalance and anterior shoulder stretches, with supervised physiotherapy. This approach is usually successful but may need to be augmented with judicious use of subacromial corticosteroid injections to settle acute symptoms in florid cases.
Knee Injection Techniques and Indications
Aspirating or injecting the knee is an important part of general practice, rheumatology, sports medicine and Orthopaedic practice. Its application not only helps confirm certain diagnoses but also allows treatment of conditions such as inflammation of the joints and around tendons. Corticosteroid injections do not slow down or change the progression of arthritis. The technique and the indications are discussed below.
Short or long acting local anaesthetics can be injected into the knee and are useful to exclude or confirm certain diagnoses. They can be used alone or mixed with corticosteroid. Toxic doses are unlikely to be exceeded in general practice but if you are in doubt consult the product information sheet. Always avoid the use of adrenaline on extremities (digits) as it can cause vasoconstriction and gangrene.
Indications Arthritic symptoms not severe enough to warrant a total knee replacement and are also useful in patients who are not medically fit for surgery.
How Long Does It Last?
The effects can take 24-48 hours to work and initially there can actually be a slight increase in pain as the corticosteroid starts to work. The effects can last anywhere from a week to 6 months but are only temporary. You can repeat the injections if required (up to three a year).
Contraindications and Side Effects Suspected infection in the joint, cellulitis, immunosuppression, allergy to local anaesthetic or steroids, joint replacement. Risk of infection is very low (1 in 5000), skin discoloration, fat necrosis, flare up of symptoms for a day or two, rise in sugar levels in diabetics (need to monitor levels carefully for about two days).Technique (performed in the office using aseptic techniques)
The choice of steroid varies. Celestone is one of the more common steroids used. Mix 2 ampoules of Celestone with 3 mls of local anaesthetic (lignocaine) in a 5ml syringe and use a blue or green (21,23G) needle. Various injection portals can be used depending on your experience. To aspirate the knee use the superolateral portal (under the patella on the lateral side with the knee extended). To inject the knee use either the inferomedial or inferolateral soft part of the knee (with the knee flexed to 90 degrees). Always use aseptic techniques. You do not need to aspirate the knee first unless there is a large effusion. If you do aspirate the knee it is best to send this for microbiological analysis.
Another part of the knee which may need to be aspirated or injected is the prepatella bursa. This is superficial and anterior to the patella and can be traumatic (housemaids knee) or infective. If you wish to aspirate this bursa because you think it is infected angle the needle straight down toward the patella with the patient lying down (and not into the knee joint itself). Using this technique if you insert your needle too far in you will hit the patella rather than entering and infecting the joint.
Other bursa or fluid collections do occur. Aspiration or injection should only be done if you are sure of the diagnosis. Otherwise it is advisable to seek an Orthopaedic opinion. A Bakers cyst is extremely common and should not generally be aspirated.
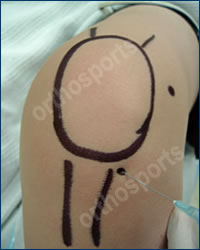
Inferolateral Portal
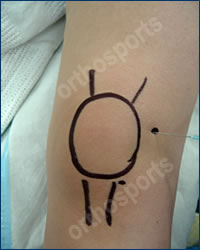
Lateral Portal
Adhesive Capsulitis occurs in people over the age of 40 years and is seen far more commonly in women than in men. It commonly occurs in diabetics and people with thyroid disease. The cause of this condition is UNKNOWN. It generally occurs spontaneously without any trauma, but can also occur after a significant traumatic event such as a fall, fracture or dislocation. The condition is also seen not infrequently after heart surgery, breast surgery or neurosurgery.
This condition commonly causes shoulder stiffness as well as pain with movements of the arm and significantly pain at night. The inside of the shoulder, the capsule, becomes inflamed and contracted. As a general rule the condition is SELF LIMITING. It can, however, take up to two years for the condition to resolve.
The condition involves three distinct phases…
- Freezing Phase or painful phase that lasts 2 to 9 months (sometimes even longer in diabetics). Patients get pain at rest and with activity, as well as pain at night. There is significant loss of motion.
- Frozen Phase – this is the progressive stiffness phase that lasts 3 to 12 months. Pain occurs only at the extremes of motion but the shoulder remains stiff.
- Thawing Phase – this is the resolution phase where movements improve over a 2 to 6 month period.
In 80% of cases the pain resolves but some patients are left with a small and permanent restriction in range of motion. This hardly ever worries the patient. Similar symptoms are caused by arthritis of the shoulder and that is the reason I order a plain x-ray in all cases. Ultrasounds and MRIs are not usually helpful.
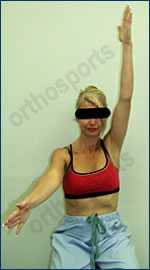
Active Forward Elevation
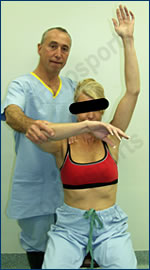
Passive Forward Elevation
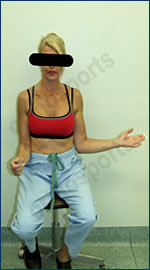
Active External Rotation
The patient exhibits significant loss of both active AND passive movements, in all directions.
TreatmentI recommend regular antiinflammatory tablets and simple analgesics. Hydrocortisone injections into the joint are an option but rarely work. At best they tend to give short lived and partial relief of symptoms. If you elect to prescribe hese injections then these should be given by a Radiologist, under Ultrasound guidance and using a sterile technique.
Physiotherapy for instruction in a gentle course of range of motion exercises is recommended. These exercises can be painful and should not include stretching exercises. The aim of the exercises is to keep the shoulder mobile and avoid further stiffness but the exercises do not improve range of motion. It is only necessary to see the physiotherapist once and the patient should perform the exercises daily.
There is a technique available called ydrodistention where a Radiologist, under Ultrasound guidance, distends the shoulder joint with fluid and breaks down the contractures. There have been reports of success with this technique leading to a more rapid recovery from the condition but there has not been a study to determine whether the results, in the long term, are any better than the “wait and see” approach.
Our advice in most cases is that the patient should learn to live with the condition for 12 to 24 months providing the pain is tolerable and the patient can cope with the activities of daily living.
If the patient has not reached the Second “FROZEN” phase within 9 to 12 months then there is a reasonable case to perform a Manipulation under Anaesthetic and an injection of cortisone. This requires an admission to hospital and a general anaesthetic. We manipulate the shoulder and inject cortisone under sterile conditions. Following the procedure the patient will require 3 to 4 months of physiotherapy. The success rate of the procedure is 70%.
In the unlikely event that the condition becomes chronic which it does in approximately 20% of people and a manipulation is unsuccessful, then we would recommend a procedure called an Arthroscopic Capsular Release to release the contracted tissue. This is a rather painful procedure that takes 6 months to recover from and requires aggressive physiotherapy following surgery. The success rate of the surgery is about 70%.There are a number of patients, who for work or social reasons, cannot afford to have a stiff shoulder for a prolonged period of time. Should that be the case then they may wish to consider having a Manipulation under Anaesthetic or a hydrodistention early in the course of the disease.
Osteotomy of the Knee
Osteotomy literally means cutting of bone. During an osteotomy the bone is cut and its position is changed in order to shift the pressures from one part of a joint to another. It is done for arthritis affecting only one side of the joint or for instability in certain situations. The idea is that the bone is cut and realigned to take pressure off the affected part and put onto a better part of the joint (hopefully taking away the pain). More recently it has been used to treat certain types of knee instability or in combination with cartilage grafting procedures.
Indications
- Patients are generally young (under 55 years of age) and active.
- They have arthritis affecting one part of the joint or malalignment or instability.
- They have a good range of motion of the joint and good bone quality.
- They are able to non weight bear on crutches and are committed to rehabilitation.
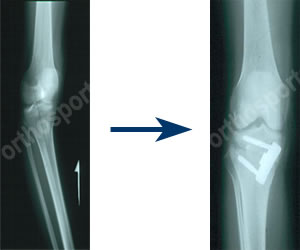
There are several good reasons to perform an HTO (High Tibial Osteotomy)…
- There is a high incidence of medial compartment osteoarthritis in physiologically young, active patients, for whom TKR is an imperfect long-term solution.
- HTO imposes no permanent activity restrictions (unlike a TKR).
- The patient is not significantly restricted with contemporary fixation (not requiring several weeks of postoperative cast immobilization as was previously needed).
- Chondral resurfacing techniques are contraindicated in the presence of tibiofemoral malalignment.
- Combining HTO with chondral resurfacing procedures may provide better results than would HTO alone.
- Many types of instability can now be treated with an osteotomy.
- In general, it is better to perform the osteotomy early (when there is less than 5 degrees of varus) and to overcorrect by 2 to 3 degrees.
Orthopaedic Surgeons and their Interests
Dr Warwick Bruce – HIP AND KNEE M.B., B.S.(Syd), F.I.C.S., F.R.A.C.S., F.A. Ortho. A.
Fellowships in Sports medicine and reconstructive hip and knee surgery. Travelling fellow in USA in joint replacement surgery. He consults at all Orthosports rooms ,operates at Calvary Hurstville Community Hospital, Canada Bay Private Hospital and Concord Hospital. He has published and written extensively and has been on the design team for hip and knee replacements.
Dr Jerome Goldberg – SHOULDER M.B., B.S., F.R.A.C.S., F.A. Ortho. A.
Fellowship at the New York Orthopaedic hospital. Special interests include arthroscopic instability and rotator cuff surgery. He consults at all Orthosports rooms, operates at Calvary Hurstville Community Hospital, Canada Bay Private Hospital and Prince of Wales Private Hospital.
Dr Andreas Loefler – SPINE, TRAUMA, HIP AND KNEE B.S.C., M.B., B.S., F.R.A.C.S. (Ortho.)
Anzac travelling fellowship of the Australian Orthopaedic Association. He consults at the Hurstville and Randwick rooms and operates at Calvary Hurstville Community Hospital, Prince of Wales Private and Public Hospitals.
Dr John Negrine – ADULT FOOT AND ANKLE M.B., B.S. (Syd), F.R.A.C.S.
Sydney Orthopaedic trained. US accredited Fellowship in foot and ankle surgery at Baylor University Medical Centre, Dallas Texas 1994. Member Australian, American and European Foot and Ankle Societies. He consults at all three Orthosports rooms and operates at Prince of Wales Private Hospital, Canada Bay Private Hospital and Calvary Hurstville Community Hospital.
Dr Rodney Pattinson – PAEDIATRICS M.B.B.S (1983) F.R.A.C.S (Ortho.)
Fellowship at the Hospital for Sick Children in London and Princess Margaret Rose Hospital in Edinburgh. He also operates on adults with hip and knee conditions. He consults at all Orthosports rooms, operates at Canada Bay Private Hospital and Sydney Children’s Hospital and St George Hospital.
Dr Ivan Popoff – SHOULDER, KNEE AND ELBOW BPhEd(1987), MBChB(1991), F.R.A.C.S. (Ortho.)
Fellowship in Sports Medicine, Shoulder and Knee Surgery, Dalhousie University, Halifax NS Canada. He consults at all the Orthosports rooms and operates at Calvary Hurstville Community, Prince of Wales Private and Canada Bay Private Hospitals.
Dr Doron Sher – KNEE, SHOULDER AND ELBOW M.B., B.S. (NSW), M.Biomed.E., F.R.A.C.S. (Ortho.)
Fellowships in upper and lower limb surgery. Sports Medicine Knee and Shoulder Surgery- Canada, Elbow surgery-Mayo Clinic, Upper Limb Surgery- New York. He consults at the Randwick and Burwood rooms and operates at Prince of Wales Private, Concord Public and Canada Bay Private Hospitals.
Dr Allen Turnbull – HIP AND KNEE M.B., B.S. (1980), F.R.A.C.S. (Ortho. 1988)
Fellow in joint replacement surgery. Interest in sporting injuries involving the knee and joint replacement. He consults at the Hurstville office. He operates at Calvary Hurstville Community Hospital, Kareena and St George Private Hospitals and St George Public Hospital.
Dr Peter Walker – HIP AND KNEE M.B., B.S. (Hons 1990), F.R.A.C.S. (Ortho.)
Awarded Zimmer travelling fellowship.Two accredited fellowships in hip and knee surgery in Boston and Toronto. He consults at the Burwood and Randwick rooms and operates at Canada Bay Private Hospital, Prince of Wales Private, Concord and Canterbury Public Hospitals.
Dr Craig Waller – HIP AND KNEE M.B., B.S. (Hons, NSW 1982), F.R.C.S. (Ed.), F.R.A.C.S. (Ortho. 1989)
He was awarded the University medal and graduate prize in surgery. He consults at the Burwood and Randwick rooms and operates at Canada Bay Private Hospital and Prince of Wales Private Hospital.
Dr John Best B.Med., Dip. Sports Med. (London), F.A.C.S.P. Sports Physician
Dr Hugh Hazard M.B., B.S., Grad. Dip. Sp. Science, F.A.C.S.P. Sports Physician
Dr Mel Cusi M.B., B.S., Cert. Sports Medicine (RACGP), F.A.C.S.P. Sports Physician
Dr Angus Bathgate M.B., B.S. Sports Physician
Dr Paul Annett M.B., B.S. (Hons. I), F.A.C.S.P. Conjoint lecturer UNSW
