Question for Physiotherapists

Proximal Hamstring Tendonopathy
Welcome to Question for Physiotherapists April 2026. This month Dr Paul Annett discusses localised buttock pain and proximal hamstring tendonopathy.
Save the Date: Saturday, 1st August 2026 for the 2026 Orthopaedic Update at UNSW and via webinar, invitations coming soon!
If you have a Question that you would like us to answer or have a colleague that would like to be included on our mailing list please email: education@orthosports.com.au
On history the patient generally has well localized pain to the ischial tuberosity, and this is typically worsened by periods of prolonged sitting, especially on hard surfaces and particularly when driving. It is more likely to cause symptoms with walking up hills and stairs rather than on the flat, and running is typically the most provocative activity.
Examination findings may include pain on lumbar flexion. Double or single pelvic bridging may provoke pain, as may resisted knee flexion (hamstring curl), with associated weakness. Direct palpation to the ischial tuberosity may cause tenderness, but the degree can be underwhelming. Examination also needs to exclude other potential causes of buttock pain, including lumbar radiculopathy, sacroillitis or hip joint pathology.
Imaging may include plain Xray, ultrasound or MRI. Xray is a useful test to assess for degenerative hip or sacroiliac disease, pelvic stress fracture or unexpected nasty pathology. Ultrasound can demonstrate thickening or calcification of the proximal hamstring tendon, but does lack accuracy when compared to MRI. MRI is much better at demonstrating tendonopathy with associated partial tearing. It can also assess for other soft tissue abnormalities such as ischiofemoral impingement. The scan will also address possible bone or joint pathology such as a sacral or pelvic stress fracture or hip or SIJ degenerative change.
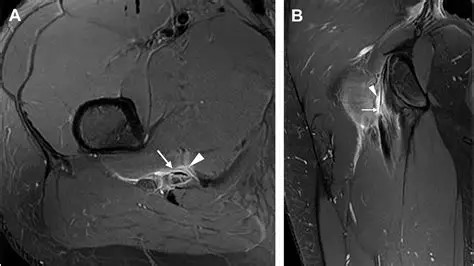
The management of proximal hamstring tendonopathy is similar to that of other tendinopathic conditions. Confirmation of diagnosis is an essential first step, whether that be from textbook clinical findings or with supportive imaging. A period of unloading is essential. This is typically an issue in runners where load needs to be reduced. This may include reduced volume, intensity and avoiding stressors such as hills and stairs. Appropriate manual therapy needs to be commenced around the hamstring, buttock and lumbar spine. Rehabilitation exercises should also be started and graded from isometric to eccentric and concentric hamstring strengthening and addressing any gluteal weakness and loss of pelvic stability.
Interventional therapy is generally injection based including both cortisone or PRP. Cortisone may be indicated in cases with more acute inflammation, such as ischial bursitis or peri-tendinitis, where the structure of the tendon is still maintained. In cases of more significant tendonopathy, especially including partial or intra-substance tears, then PRP is a preferred alternative. Whilst there are limited studies regarding this, one suggested 68% of patients improved by more than a 50% reduction in pain after a single injection(1). Surgery is typically not indicated unless there is a complete disruption of the tendon attachment or protracted symptoms resistant to other appropriate treatment modalities.

Reference:
1. Platelet-rich plasma for treatment of chronic proximal hamstring tendinopathy, April 2020, Regen Med

Tumours of the foot & ankle
Welcome to Question for Physiotherapists March 2026. This month Dr John Negrine discusses tumours of the foot & ankle. Save the Date: Saturday, 1st August 2026 for the 2026

Knee Injuries from bouldering
Welcome to Question for Physiotherapists February 2026. This month Dr Doron Sher discusses Complex Knee Injuries from Bouldering. Save the Date: 2026 Orthopaedic Update will be held Saturday,

Syndesmosis Injury
Welcome to Question for Physiotherapists November 2025. This month Dr John Negrine discusses syndesmosis injury. If you registered for the Orthopaedic Updates Webinar 2025 the recorded webinar will

Acromioclavicular (AC) Joint Injuries
Welcome to Orthosports Question for Physiotherapists October 2025. This month Dr Doron Sher discusses acromioclavicular joint injuries. Reminder to Register Orthosports Annual Orthopaedic Updates, Saturday, 8th November, 2025
Wrist Fracture Xrays
Welcome to Orthosports Question for Physiotherapists August 2025. This month Dr Kwan Yeoh discusses wrist fractures and xrays. REGISTRATIONS OPEN Orthosports Annual Orthopaedic Updates, Saturday, 8th November, 2025, to register
NRL head injury management
Welcome to Orthosports Question for Physiotherapists June 2025. This month Dr Paul Annett discusses the NRL decision making behind the head injury process. REMINDER: SAVE THE DATE Orthosports Annual

Internal Impingement of the Shoulder
Welcome to Orthosports Question for Physiotherapists May 2025. This month Dr Leigh Golding discusses internal impingement of the shoulder. REMINDER: SAVE THE DATE Orthosports Annual Orthopaedic Updates, Saturday, 8th
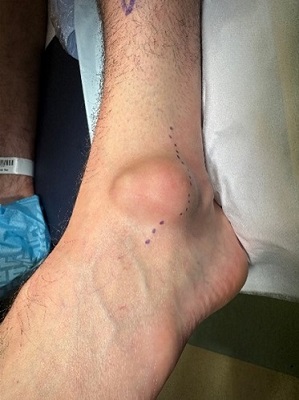
Swollen Ankle
Welcome to Orthosports Question for Physiotherapists April 2025. This month Dr John Negrine discusses a swollen ankle. REMINDER: SAVE THE DATE Orthosports Annual Orthopaedic Updates, Saturday, 8th November, 2025,

Glenoid track and shoulder instability scoring system
Welcome to Orthosports Question for Physiotherapists March 2025. This month Dr Doron Sher gives an update on the glenoid track and shoulder instability scoring system. Do you

Spontaneous Osteonecrosis
Welcome to Orthosports Question for Physiotherapists September 2024. This month Dr Doron Sher discusses Spontaneous Osteonecrosis. REMINDER TO REGISTER Orthosports Annual Orthopaedic Updates, Saturday, 9th November 2024, Live event
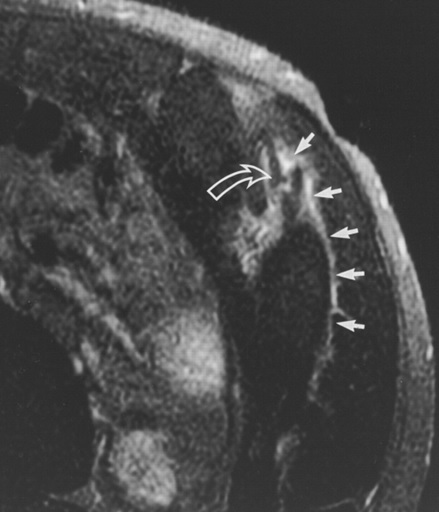
Side Strain
Welcome to Orthosports Question for Physiotherapists August 2024. This month Dr Leigh Golding discusses side strain from a sporting injury. REMINDER: SAVE THE DATE Orthosports Annual Orthopaedic Updates, Saturday,
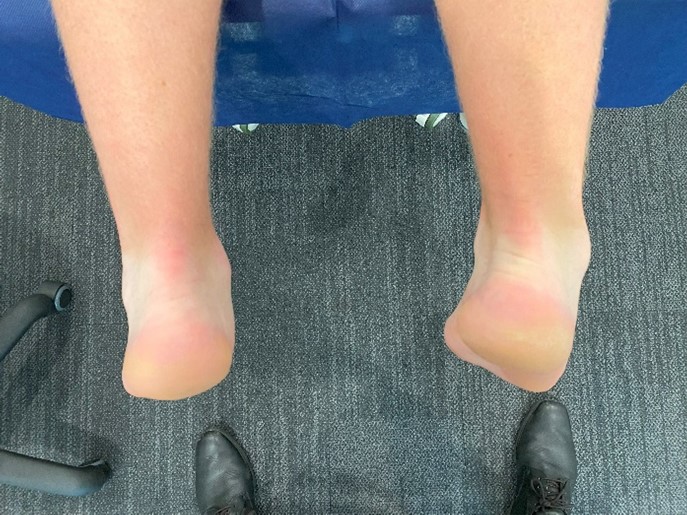
Tarsal coalition
Welcome to Orthosports Question for Physiotherapists July 2024. This month Dr Paul Annett discusses Tarsal coalition. REMINDER: SAVE THE DATE Orthosports Annual Orthopaedic Updates, Saturday, 9th November 2024, live

Patella dislocation
Welcome to Orthosports Question for Physiotherapists May 2024. This month Dr Doron Sher discusses Patella dislocation SAVE THE DATE: Orthosports Annual Orthopaedic Updates, Saturday, 9th November 2024, live
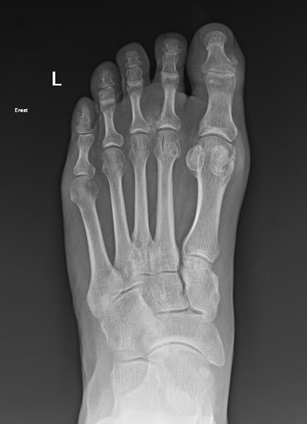
Gout
Welcome to Orthosports Question for Physiotherapists April 2024. This month Dr John Negrine discusses the common condition of Gout. SAVE THE DATE: Orthosports Annual Orthopaedic Updates, Saturday, 9th
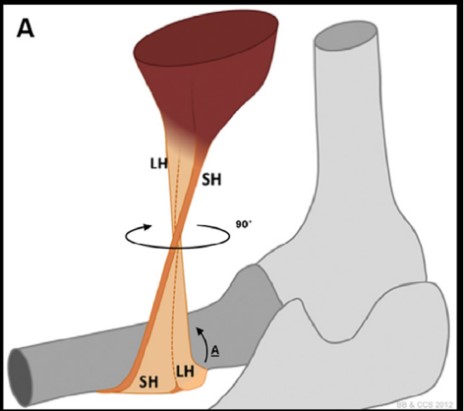
Distal Biceps Rupture
Welcome to Orthosports Question for Physiotherapists February 2024. This month Dr Doron Sher discusses management of distal biceps rupture. If you have a Question that you

Sport after Total Knee Replacement
Welcome to Orthosports Question for Physiotherapists, October 2023. This month Dr Doron Sher discusses return to sport after total knee replacement. REMINDER: Register your place for the Annual Orthopaedic Updates.

High Tibial Osteotomy and Uni Knee Replacement
Welcome to Orthosports Question for Physiotherapists, September 2023. This month Dr Doron Sher discusses the comparison of the High Tibial Osteotomy vs the Unicompartmental Knee Replacement. Register your

Achilles Tendon Ruptures
Welcome to Orthosports Question for Physiotherapists, August 2023. This month Dr John Negrine discusses Achilles Tendon Ruptures. Save the Date: Saturday, 4th November, 2023 Annual Orthopaedic Updates. Live

Lateral extra-articular tenodesis
Welcome to Orthosports Question for Physiotherapists, June 2023. This month Dr Michael Goldberg discusses lateral extra-articular tenodesis and why you would add this procedure to an ACL

Adding a Patch to Rotator Cuff Repairs
Welcome to Orthosports Question for Physiotherapists, May 2023. This month Dr Doron Sher discusses the use of a patch in Rotator Cuff Repairs. Save the Date: Saturday, 4th

Imaging for ACL Injury
Welcome to Orthosports Question for Physiotherapists, October 2022. This month Dr Doron Sher discusses imaging for a suspected ACL injury. Save the Date: Saturday, 12 November, 2022 Annual

Glenoid Track and Shoulder Instability
Welcome to Orthosports Question for Physiotherapists August, 2022. This month Dr Doron Sher discusses a question on the glenoid track and shoulder instability. Please send your Questions

OSTEOCHONDRITIS DISSECANS
Welcome to Orthosports Question for Physiotherapists May, 2022. This month Dr Doron Sher discusses a question on treatment options for an OCD Lesion. Save the Date: Saturday,

Accessory Bones of the Foot and Ankle
Welcome to Question for Physiotherapists, April, 2022 This month Dr John Negrine discusses accessory bones of the foot and ankle. Please feel free to send your

Hypermobile Lateral Meniscus
Welcome to Question for Physiotherapists, March, 2022 This month Dr Michael Goldberg discusses the Hypermobile Lateral Meniscus. Please feel free to send your questions to
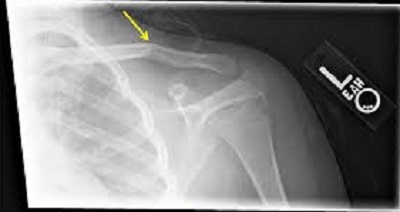
Imaging in Musculoskeletal assessment
Welcome to Question for Physiotherapists, February, 2022 This month Dr Paul Annett discusses Imaging inMusculo-skeletal Assessment. Please feel free to send your questions to education@orthosports.com.au Dr

Shoulder Injury related to vaccine administration
Welcome to Question for Physiotherapists, January, 2022 This month Dr Doron Sher discusses Shoulder Injury related to Vaccine administration. Please feel free to send your questions

Chondral Grafting in the knee
Welcome to Question for Physiotherapists, November 2021. This month Dr Doron Sher discusses Chondral Grafting in the knee.Please feel free to send your questions to education@orthosports.com.au CHONDRAL
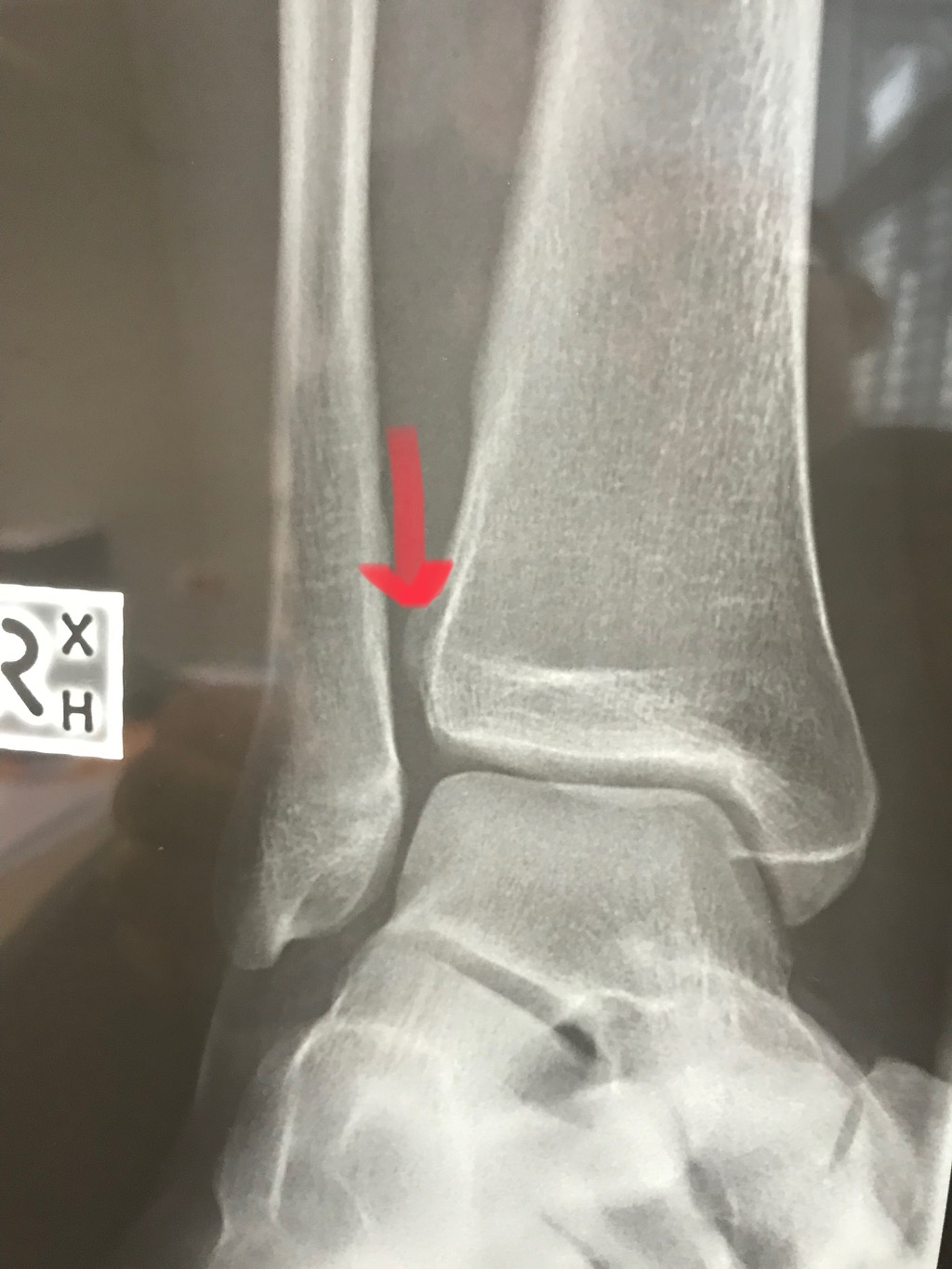
Syndesmosis Fixation
Welcome to Question for Physiotherapists, October 2021. This month Dr Todd Gothelf discusses Syndesmosis fixation. Please feel free to send your questions to education@orthosports.com.au QUESTION I
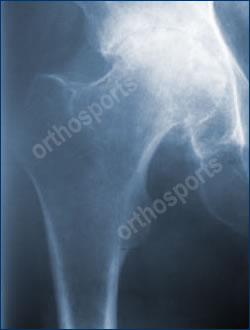
Hip Precautions following Total Hip Replacement
Welcome to Question for Physiotherapists, September 2021. This month Dr Christopher Spelman discusses precautions after a Total Hip Replacement. Please feel free to send your questions
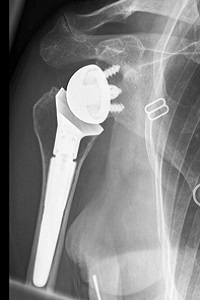
Reverse Shoulder Replacement Rehabilitation
Welcome to Question for Physiotherapists, August 2021. This month Dr Doron Sher discusses rehabilition after a Reverse Shoulder Replacement. Please feel free to send your questions
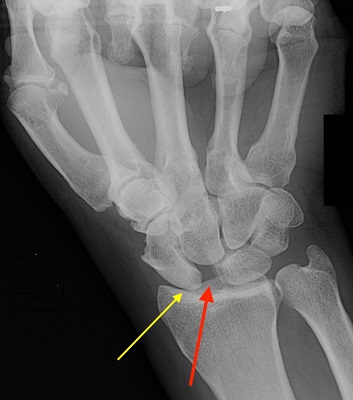
Chronic Scapholunate Ligament Rupture
Welcome to Question for Physios, July 2021. This month Dr Kwan Yeoh discusses the management of Complete Scapholunate Ligament Rupture. Please feel free to send your
Assessing Sports Injury
Welcome to Question for Physiotherapists June 2021. This month Dr Paul Annett presents an article on assessing a patient that presents with potentially more than a
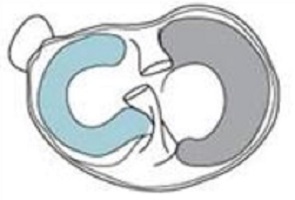
Discoid Lateral Meniscus
Welcome to Question for Physiotherapists May 2021. This month Dr Doron Sher presents an article on a Discoid Lateral Meniscus. Please feel free to send
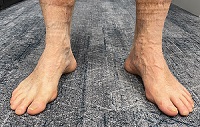
Cavo-Varus (High Arched) Feet
QUESTION | Why are high arched feet more interesting than flat feet? ANSWER | A 43 year old man presents with numbness on the outer
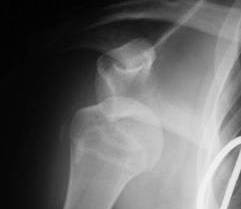
Surgical Treatment of Unstable Shoulder
QUESTION | | Surgical treatment of the unstable shoulder – How do you decide which patient gets what operation? We know that younger patients and those
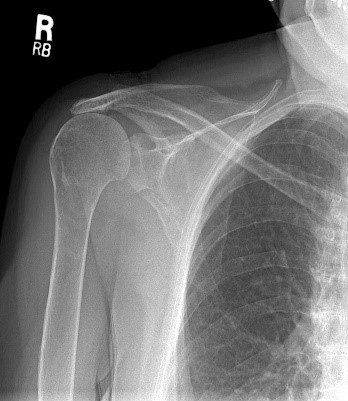
Full Thickness Tear of Supraspinatus Tendon
QUESTION | My patient is a 67 year old female who has had pain during overhead activity (catching pain), going on for over 5 years.
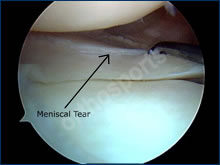
Medial Meniscal Root Tears
QUESTION I I have a patient in her 50s who has had a meniscus repair done. I thought that the studies showed no advantage when doing
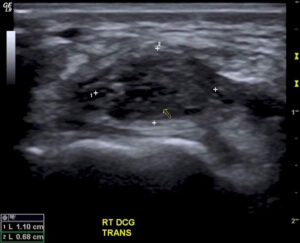
Wrist Ganglion & Carpal Instability
QUESTION| How Does a Wrist Ganglion relate to Carpal Instability? How is it best treated? ANSWER | A ganglion is a benign synovium-lined cystic collection of
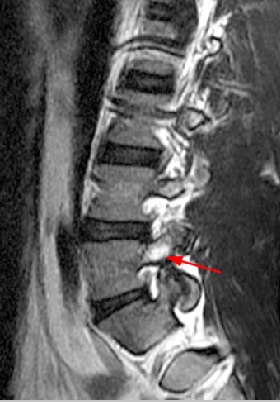
Lumbar Stress Fractures
QUESTIONS | 1. What is rest in treatment of stress fracture? Walking only? Bike? Swim(in non-extended position)? What can you do? Or is it just not
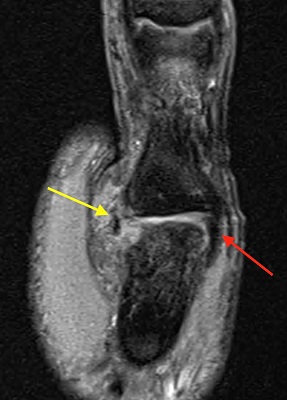
Collateral Ligament Tear
QUESTION | WHEN DOES A COLLATERAL LIGAMENT TEAR OF THE THUMB NEED SURGERY? ANSWER | For the purposes of this question, I’m going to assume

Distal Biceps Rupture
QUESTION | I recently had a patient with a partial distal biceps rupture. Why was he offered surgery without trying non-operative management? ANSWER | Anatomy:
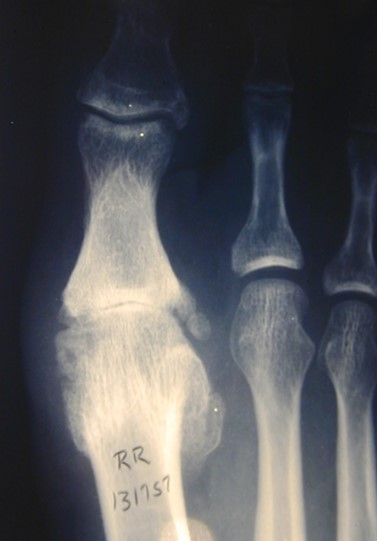
Hallux Rigidus
QUESTION | What are the best options for a 50 year old runner with Hallux Rigidus? ANSWER | A 50 year old runner with hallux
Previous Question for Physiotherapists:
| Dec-2020 | Wrist Ganglions | Dr Kwan Yeoh |
| Oct/Nov-2020 | Medial Meniscal Root Tears | Dr Doron Sher |
| Sep-2020 | Lumbar Stress Fractures | Dr Paul Annett |
| Aug-2020 | Frailty and Healthy Ageing | Dr John Best |
| Jul-2020 | Thumb – Collateral Ligament Tear | Dr Kwan Yeoh |
| Jun-2020 | Shoulder Instability | Dr Doron Sher |
| May-2020 | Hallux Rigidus | Dr John Negrine |
| Mar/Apr-2020 | Achilles Tendon Ruptures | Dr Todd Gothelf |
| Feb-2020 | Distal Biceps | Dr Doron Sher |
| Nov-2019 | Clavicle Fracture Internal Fixation | Dr Doron Sher |
| Oct-2019 | Femoracetabular Impingement (FAI) | Dr Paul Mason |
| Sep-2019 | Imaging for Acute ACL Injuries | Dr Doron Sher |
| Aug-2019 | Joint Relocation | Dr Paul Annett |
| Jul-2019 | Guyon canal surgery | Dr Kwan Yeoh |
| Jun-2019 | Whats new in ACL reconstruction 2019 | Dr Doron Sher |
| May-2019 | Cuneiform Fracture | Dr Todd Gothelf |
| Apr-2019 | Flexor Tendon Injuries | Dr Kwan Yeoh |
| Mar-2019 | Chronic Exertional Compartment Synd | Dr Paul Annett |
| Feb-2019 | Achilles Tendon Rupture | Dr John Negrine |
| Nov-2018 | Low Back Pain | Dr Paul Mason |
| Sep-2018 | Concussion part 2 | Dr John Best |
| Jul-2018 | Concussion part1 | Dr Paul Annett |
| Jun-2018 | Thessaly & McMurray Test | Dr Doron Sher |
| May-2018 | AC Joint | Dr Doron Sher |
| Apr-2018 | Arthritis of the fingers | Dr Kwan Yeoh |
| Feb-2018 | CLAVICLE fractures | Dr Doron Sher |
| Oct-2017 | ACL Grafts | Dr Doron Sher |
| Sep-2017 | Forefoot pain | Dr John Negrine |
| Aug-2017 | Wrist Ganglion | Dr Kwan Yeoh |
| Jul-2017 | Anterolateral Ligament Reconstruction | Dr Doron Sher |
| Jun-2017 | Scapholunate ligament | Dr Kwan Yeoh |
| Apr-2017 | Knee Brace – ACL Reconstruction | Dr Doron Sher |
| Mar-2017 | Sesamoid fractures | Dr Kwan Yeoh |
| Feb-2017 | Plantar Fasciitis | Dr Todd Gothelf |
| Nov-2016 | Sternoclavicular Joint | Dr Doron Sher |
| Oct-2016 | Proximal Humerus Fractures | Dr David Lieu |
| Sep-2016 | Wrist Fractures | Dr Kwan Yeoh |
| Aug-2016 | Patella Instability | Dr Doron Sher |
| Jul-2016 | Snowboarders ankle | Dr Todd Gothelf |
| May-2016 | Cortisone Injections | Dr Paul Annett |
| Apr-2016 | Shoulder Instability_1 | Dr Ivan Popoff |
| Mar-2016 | Exercise after TKR | Dr Doron Sher |
| Dec-2015 | Scaphoid OA | Dr Kwan Yeoh |
| Nov-2015 | Greater Tuberosity Fractures | Dr Doron Sher |
| Oct-2015 | Stress Fractures | Dr Paul Annett |
| Sep-2015 | Boxers Fractures | Dr Kwan Yeoh |
| Aug 2015 | Resistance Training | Dr John Best |
| July 2015 | LARS Ligament | Dr Ivan Popoff |
| Jun-2015 | Distal Biceps | Dr Doron Sher |
| May-2015 | Latarjet procedure | Dr Jerome Goldberg |
| Apr-2015 | TFCC Questions | Dr Kwan Yeoh |
| Mar-2015 | Acute Ankle Sprains | Dr Todd Gothelf |
| Nov-2014 | PRPP | Dr Paul Annett |
| Oct-2014 | Driving After Surgery | Dr Doron Sher |
| Sep-2014 | Distal Biceps Rupture | Dr Doron Sher |
| Aug-2014 | Ankle Sprain | Dr Todd Gothelf |
| Jun-2014 | Patella Dislocation | Dr Doron Sher |
| May-2014 | Shoulder Instability | Dr Todd Gothelf |
| Apr-2014 | De Quervains | Dr Kwan Yeoh |
| Mar-2014 | Acromio-clavicular joint injuries | Dr Todd Gothelf |
| Feb-2014 | Chronic Knee Pain | Dr Paul Annett |
| Dec-2013 | Foot and Ankle Questions | Dr John Negrine |
| Oct-2013 | Rotator Cuff Repair | Dr Todd Gothelf |
| Sep-2013 | ACL Reconstruction | Dr Doron Sher |
| Jul-2013 | Slipped Upper femoral epiphysis | Dr Rod Pattinson |
| May-2013 | Skiers thumb | Dr Kwan Yeoh |
| Apr-2013 | Bakers_Cyst | Dr Ivan Popoff |
| Mar-2013 | Tibial Osteotomy vs UKR | Dr Doron Sher |
| Feb-2013 | ALIF success rate | Dr Andreas Loefler |
| Jan-2013 | Lisfranc Injuries | Dr Todd Gothelf |
| Nov-2012 | Anterior Spinal Fusions | Dr Andreas Loefler |
| Oct-2012 | MCL Injuries | Dr Doron Sher |
| Sep-2012 | Compartment Syndrome | DrPaul Annett |
| Aug-2012 | Carpal tunnel | Dr Kwan Yeoh |
| July-2012 | Anterior Process Calcaneus Fx | Dr Todd Gothelf |
| Jun-2012 | Tenodesis vs Tenotomy | DrJeromeGoldberg |
| May-2012 | Osteoarthritis in the young active patient | Dr Doron Sher |
| Apr-2012 | Syndesmosis Sprain | Dr Todd Gothelf |
| Mar-2012 | Triangular Fiocartilage Injuries | Dr Kwan Yeoh |
| Jan-2012 | Shoulder Replacement Older Population | Dr Jerome Goldberg |
| Dec-2011 | Wrist Fracture | Dr Kwan Yeoh |
| Nov-2011 | Adductor Tendon Tear | Dr Paul Annett |
| Oct-2011 | Navicular Pain | Dr Todd Gothelf |
| Sep-2011 | OCD Lesion | Dr Doron Sher |
| Aug-2011 | Metal on Metal Hip Replacements | Dr Andreas Loefler |
| July-2011 | Femoral Neck Stress Fract (Pt 2) | Dr John Best |
| Jun-2011 | Femoral Neck Stress Fractures | Dr John Best |
| May-2011 | PCL Injury Part 2 | Dr Doron Sher |
| Apr-2011 | PCL Injury Part 1 | Dr DoronSher |
| Mar-2011 | Prolotherapy Autologous Blood Injections | DrPaul Annett |
| Feb-2011 | Shoulder Impingement | Dr Todd Gothelf |
| Dec-2010 | Does Chondral Grafting Work | DrDoron Sher |
| Nov-2010 | Shoulder Immobilisation-Dislocation | Dr Jerome Goldberg |
| Sep-2010 | SLAP Lesions Stable Shoulder | Dr ToddGothelf |
| Jul-2010 | Ankle Sprains | Dr Todd Gothelf |
| Jun-2010 | Dislocation After THR | Dr Peter Walker |
| May-2010 | Acupuncture Muscle Strength Programmes | Dr Paul Annett |
| April-2010 | Full Thickness Rotator Cuff Tears | Dr JeromeGoldberg |
| Mar-2010 | Skiing after TKR | Prof Warwick Bruce |
| Feb-2010 | Fractures of the Clavicle | Dr John Trantalis |
| Jan-2010 | Osteoarthritis of the Knee | Dr Doron Sher |
| Dec-2009 | Fifrth Metatarsal Fractures | Dr Todd Gothelf |
| Nov-2009 | Partial Rotator Cuff Tears | Dr Todd Gothelf |

